Vision plays a central role in maintaining independence and quality of life, especially in older adults. Among age-related eye conditions, cataracts are one of the most common yet treatable causes of visual impairment. In geriatric care, cataracts are not viewed as an isolated eye issue but as a condition that can significantly influence mobility, safety, and overall well-being.
At Liv Hospital, specialists approach cataracts through a comprehensive geriatric lens—focusing not only on restoring vision but also on preserving functional independence. To learn more about this condition, you can explore GERIATRICS Overview and Definition and how modern medicine addresses cataracts in older adults.
What Is a Cataract?
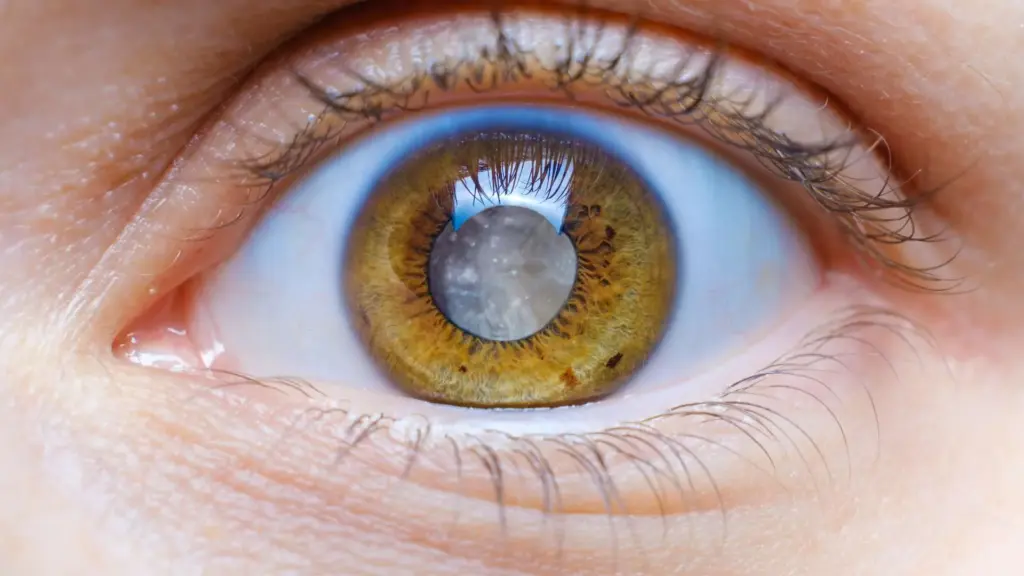
A cataract occurs when the natural lens of the eye becomes cloudy over time. This lens is normally clear and helps focus light onto the retina to produce sharp images. However, as we age, changes in lens proteins cause it to lose its transparency.
This gradual clouding interferes with how light enters the eye, leading to blurred or dim vision. Unlike sudden eye conditions, cataracts typically develop slowly, which is why many people may not notice the changes immediately.
Why Cataracts Matter in Geriatrics
In older adults, vision impairment has far-reaching consequences beyond eyesight. Reduced visual clarity can affect balance, coordination, and confidence in daily activities.
Cataracts are particularly important in geriatric care because they are closely linked to:
- increased risk of falls and injuries
- reduced ability to perform daily tasks
- social withdrawal due to limited mobility
- decreased overall quality of life
Addressing cataracts early helps prevent these secondary complications and supports healthy aging.
How Cataracts Develop Over Time
Cataracts are primarily associated with aging, but their development is influenced by multiple biological and environmental factors. Over time, oxidative stress and metabolic changes alter the structure of lens proteins, causing them to clump together.
As the condition progresses:
- the lens gradually becomes more opaque
- light transmission decreases
- visual clarity continues to decline
This process can take years, with symptoms slowly worsening if left untreated.
Common Types of Cataracts in Older Adults
Not all cataracts develop in the same way. In geriatric patients, doctors typically identify different types based on where the clouding occurs within the lens.
- Nuclear cataracts form in the center and are often linked to aging
- Cortical cataracts develop around the edges and may cause glare or light sensitivity
- Posterior subcapsular cataracts appear at the back of the lens and can affect vision more rapidly
Understanding the type of cataract helps guide diagnosis and treatment planning.
Recognizing Early Signs of Cataracts
Cataracts often begin with subtle symptoms that gradually become more noticeable. Many older adults describe their vision as becoming dull or hazy over time.
Common early signs include:
- blurred or cloudy vision
- increased sensitivity to light and glare
- difficulty seeing at night
- fading or yellowing of colors
- frequent changes in eyeglass prescription
Recognizing these symptoms early allows for timely evaluation and management.
The Broader Impact on Daily Life
Cataracts can significantly affect how older adults interact with their surroundings. Tasks that once seemed simple—such as reading, driving, or recognizing faces—may become challenging.
This decline in visual function can lead to:
- hesitation in movement or walking
- avoidance of social activities
- increased dependence on caregivers
- reduced confidence in performing daily routines
Because of these effects, cataract management is an important part of maintaining independence in aging populations.
The Role of Comprehensive Geriatric Care
Managing cataracts involves more than diagnosing lens opacity. Geriatric specialists consider the patient’s overall health, lifestyle, and coexisting conditions when planning care.
A comprehensive approach may include:
- evaluating other eye conditions such as glaucoma or macular degeneration
- assessing overall physical and cognitive health
- ensuring safe mobility and fall prevention
- supporting patients through decision-making and treatment options
This holistic care model ensures that treatment aligns with the patient’s broader health needs.
Looking Ahead: Vision and Healthy Aging
Cataracts remain one of the most treatable causes of vision loss, making early awareness and proper care essential. With modern medical advancements, restoring vision can significantly improve independence and quality of life for older adults.
In addition to medical care, maintaining healthy daily habits plays an important role in supporting long-term eye health. For more insights into lifestyle choices, nutrition, and wellness practices, you can visit live and feel, a platform dedicated to promoting healthier living and overall well-being.